How Is Human Papillomavirus (HPV) Diagnosed?
Written by Anoush Gomes

Anoush Gomes is a seasoned Content Writer with over 10 years of experience, specializing in various writing styles such as medical content, creative writing, storytelling, and research papers. Anoush embarked on a unique journey, starting with pre-medical studies at the Dante Aligheri Academy and the University of Miami, where she earned a Bachelor's degree with a major in Biology and a minor in Psychology.Having pursued medical school and completed clinicals, Anoush transitioned to the world of medical content writing, where her passion for both healthcare and writing converged. Her writing skills encompass persuasive, narrative, expository, and descriptive styles, making complex medical concepts accessible to diverse audiences.Beyond her professional endeavors, Anoush is a multi-faceted individual with a rich tapestry of interests. A writer, artist, poet, avid reader, certified nerd, and hopeful author, she finds inspiration in the intersection of creativity and science.Whether crafting engaging medical narratives or weaving captivating stories, Anoush combines her diverse background and writing expertise to deliver compelling content that resonates with diverse audiences.
•
May 4, 2024
Our experts continually monitor the health and wellness space, and we update our articles when new information becomes available.
Human Papillomavirus (HPV) is a widespread sexually transmitted infection (STI) with significant health implications, ranging from genital warts to various types of cancer. Timely and accurate diagnosis of HPV is paramount for effective management and prevention of associated complications. In this extensive guide, we explore in detail the diverse methods employed in diagnosing HPV infection, encompassing clinical evaluation, laboratory tests, screening procedures, advanced diagnostic technologies, and the implications of diagnosis for patients and healthcare providers. Before delving into the diagnostic methods, it's crucial to grasp the basics of HPV. Human Papillomavirus encompasses a large group of viruses, over 200 strains identified, with approximately 40 types primarily affecting the genital area. While some HPV strains cause benign conditions such as genital warts, others, notably high-risk types like HPV 16 and 18, are strongly linked to cervical, anal, and other cancers.
Clinical Evaluation
Physical Examination:
- Description: Healthcare providers conduct a thorough physical examination to identify visible signs of HPV infection, such as genital warts or abnormal skin changes.
- Scope: Examination may involve inspecting the genital and anal regions, as well as other susceptible areas like the mouth and throat.
- Detailed Inspection: During the examination, healthcare providers carefully observe for any abnormalities, noting the size, shape, colour, and texture of any lesions or growths.
Medical History Assessment:
- Description: Obtaining a detailed medical history aids in assessing risk factors and symptoms of HPV infection.
- Inquiry: Healthcare professionals inquire about sexual activity, previous STI diagnoses, vaccination history, and relevant symptoms or concerns.
- Family History: Additionally, providers may inquire about family history of HPV-related conditions or cancers, as genetic predisposition can play a role in susceptibility to certain HPV strains.
Laboratory Tests
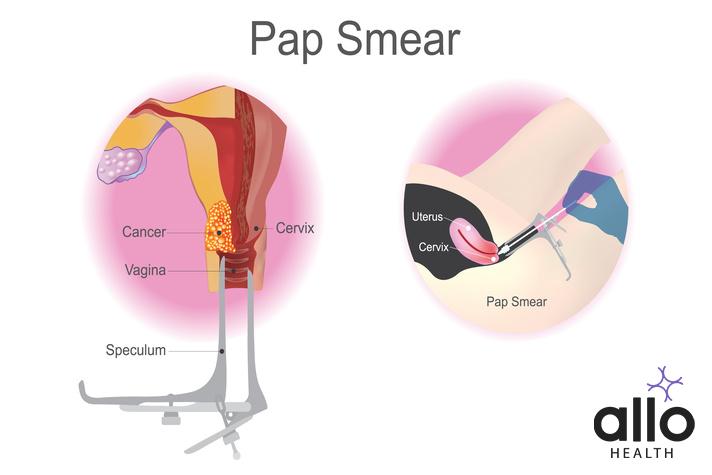
Pap Smear Test (Pap Test):
- Description: Pap smear is a screening test used to detect abnormal changes in cervical cells, indicating HPV infection or pre-cancerous conditions.
- Procedure: During a Pap smear, cells are collected from the cervix and examined under a microscope to identify any abnormalities.
- Frequency: Pap smears are typically performed every three years for individuals aged 21 to 65, although screening intervals may vary based on individual risk factors and healthcare guidelines.
HPV DNA Test:
- Description: HPV DNA testing identifies the presence of high-risk HPV strains in cervical cells, providing a sensitive method for HPV infection detection.
- Procedure: Samples of cervical cells are collected and tested for HPV DNA using molecular techniques like polymerase chain reaction (PCR) or hybrid capture assays.
- Indications: HPV DNA testing may be recommended as a primary screening tool for women aged 30 and older, in conjunction with Pap smears, or as a follow-up test for individuals with abnormal Pap smear results.
Biopsy:
- Description: In cases of abnormal findings from Pap smears or HPV DNA tests, a biopsy may be necessary to evaluate cellular changes and determine further treatment.
- Procedure: A tissue sample is collected from the affected area (e.g., cervix, genital warts) and examined under a microscope for signs of HPV-related abnormalities or cancer.
- Types: Biopsies may be performed using various techniques, including colposcopy-guided biopsy, punch biopsy, or excisional biopsy, depending on the location and size of the lesion.
Screening Procedures

Cervical Cancer Screening:
- Description: Routine cervical cancer screening aims to detect abnormal cervical cell changes early, facilitating timely intervention.
- Tests: Screening methods include Pap smears, HPV DNA testing, or a combination based on age, risk factors, and guidelines.
- Importance of Screening: Cervical cancer screening has significantly reduced the incidence and mortality of cervical cancer, making it a cornerstone of preventive healthcare for women.
Anal Cancer Screening:
- Description: Individuals at increased risk of anal cancer, such as men who have sex with men (MSM), undergo anal cancer screening to detect abnormal anal cell changes.
- Tests: Screening may involve anal Pap smears, HPV DNA testing, or high-resolution anoscopy (HRA) for further evaluation.
- Barriers to Screening: Despite the increased risk of anal cancer among certain populations, such as MSM living with HIV, anal cancer screening remains underutilised due to lack of awareness, stigma, and limited access to healthcare resources.
Oropharyngeal Cancer Screening:
- Description: Screening for oropharyngeal cancer targets individuals at high risk of HPV-related throat cancer.
- Tests: Methods may include visual examination, biopsy, or imaging tests to assess suspicious lesions or masses.
- Challenges in Diagnosis: Diagnosing oropharyngeal cancer poses challenges due to the complex anatomy of the throat and the absence of routine screening programs. As a result, many cases are diagnosed at advanced stages, highlighting the need for improved detection strategies and awareness campaigns.
Advanced Diagnostic Technologies
HPV Genotyping:
- Description: HPV genotyping identifies specific HPV strains present in a sample, providing insights into infection type and potential cancer risk.
- Applications: Used in research, epidemiological studies, and clinical settings to tailor treatment and monitor HPV infections.
- Types of Tests: HPV genotyping assays vary in complexity and target different HPV strains, ranging from simple PCR-based tests to more comprehensive multiplex assays capable of detecting multiple HPV types simultaneously.
Molecular Biomarkers:
- Description: Molecular biomarkers detect HPV-related changes in cellular DNA or RNA, aiding in early cancer detection and risk assessment.
- Emerging Technologies: Advances in biomarker research hold promise for non-invasive HPV diagnosis and personalized treatment approaches.
- Examples: Biomarkers such as p16INK4a and E6/E7 mRNA have shown promise as indicators of HPV-related cellular changes and may serve as valuable adjuncts to traditional screening methods.
Implications of Diagnosis
Psychological Impact:
- Description: Diagnosis of HPV infection, particularly in cases involving high-risk strains or precancerous lesions, can have significant psychological effects on patients.
- Emotional Response: Patients may experience feelings of anxiety, fear, or stigma associated with the diagnosis, leading to emotional distress and concerns about their future health outcomes.
- Supportive Care: Healthcare providers play a crucial role in providing emotional support, education, and resources to help patients cope with the psychological impact of HPV diagnosis and navigate the treatment process.
Treatment Considerations:
- Description: Diagnosis of HPV-related conditions, such as genital warts or cervical dysplasia, necessitates appropriate treatment interventions to manage symptoms and prevent disease progression.
- Treatment Options: Treatment modalities may include topical medications, surgical procedures, or ablative therapies, depending on the severity and location of the lesions.
- Patient Education: Healthcare providers should educate patients about treatment options, potential side effects, and the importance of adherence to follow-up care to ensure optimal outcomes.
Partner Notification and Prevention:
- Description: HPV diagnosis underscores the importance of partner notification and prevention strategies to reduce the risk of transmission and future infections.
- Communication with Partners: Patients diagnosed with HPV should be encouraged to inform their sexual partners about the infection, discuss safe sex practices, and encourage partner vaccination if appropriate.
- Preventive Measures: In addition to partner notification, preventive measures such as condom use, HPV vaccination, and regular screening are essential for reducing the burden of HPV-related diseases and preventing transmission within the community.
Accurate diagnosis of Human Papillomavirus (HPV) infection is critical for effective management and prevention of associated health complications. Clinical evaluation, laboratory tests, screening procedures, and advanced diagnostic technologies play pivotal roles in identifying HPV-related abnormalities and guiding appropriate treatment interventions. By prioritizing regular screening, early detection, and comprehensive sexual health education, individuals can take proactive steps to safeguard their health and well-being in the face of HPV infection. Moreover, healthcare providers play a crucial role in supporting patients through the diagnostic process, providing education, emotional support, and personalized care to optimize health outcomes and promote overall well-being.
Disclaimer
The following blog article provides general information and insights on various topics. However, it is important to note that the information presented is not intended as professional advice in any specific field or area. The content of this blog is for general educational and informational purposes only. The content should not be interpreted as endorsement, recommendation, or guarantee of any product, service, or information mentioned. Readers are solely responsible for the decisions and actions they take based on the information provided in this blog. It is essential to exercise individual judgment, critical thinking, and personal responsibility when applying or implementing any information or suggestions discussed in the blog.
Most Asked Questions
How is HPV diagnosed in men?
HPV diagnosis in men often involves visual inspection for genital warts and may include HPV DNA testing for high-risk strains associated with cancer. However, routine screening for HPV-related cancers in men is less common compared to women.
Can HPV be diagnosed without visible symptoms?
Yes, HPV can be diagnosed without visible symptoms through laboratory tests such as Pap smears and HPV DNA testing. These tests can detect abnormal cellular changes caused by HPV infection, even in the absence of visible warts or lesions.
What is the difference between a Pap smear and an HPV DNA test?
A Pap smear detects abnormal changes in cervical cells, while an HPV DNA test identifies the presence of high-risk HPV strains in cervical cells. Both tests are used in cervical cancer screening, with Pap smears serving as a primary screening tool and HPV DNA tests providing supplemental information for risk assessment.
At what age should individuals start getting screened for HPV?
Screening guidelines for HPV vary by country and healthcare organization. In general, cervical cancer screening with Pap smears typically begins at age 21, with HPV DNA testing added as an option at age 30 or older, or as recommended by healthcare providers based on individual risk factors.
What should I do if I test positive for HPV?
If you test positive for HPV, it's essential to follow up with your healthcare provider for further evaluation and management. Depending on the test results and any associated symptoms, your provider may recommend additional tests, treatment for visible warts or lesions, and preventive measures such as vaccination and safe sex practices.